Psoriasis
Written by Dr Claudia Pastides, 8th March 2019
Psoriasis is an autoimmune condition that affects the skin, nails and sometimes the joints. It isn’t clear why, but the body’s immune system attacks the skin and this unnecessarily increases the production of skin cells. As the production of skin cells increases, there is a build up of scaly, warm, red, itchy and occasionally painful patches on various parts of the body.
Roughly 2% of the UK population1 is estimated to have psoriasis. It is a disease that often comes and goes; managed by medication and lifestyle measures.
What does psoriasis look like?
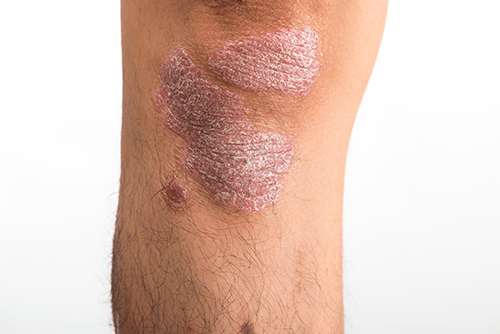
80-90% of psoriasis is “plaque psoriasis”, which typically presents as red patches of skin, larger than 0.5cm in diameter, that look slightly raised off the surface of the skin and are covered with a thick silvery crust or scale.
The rash is usually in more places than one on the body and often itchy or uncomfortable. Occasionally the skin looks cracked and bleeds.
Psoriasis is not infectious and does not spread from person to person.
There are a few other much less common types of psoriasis that present in different ways:
- Guttate psoriasis - very small pink lesions on the skin, often occurring after a throat or skin infection with Group A Streptococcus
- Pustular psoriasis - small blisters, frequently on the palms or soles
- Palmoplantar psoriasis - red scaly rash on hands and soles of feet
- Annular psoriasis - scaly round patches in the shape of a doughnut, with the centre clear
- Flexural psoriasis - the psoriasis rash is localised to skin creases (i.e. groin, armpits, under breasts) and sometimes is due to a fungal infection
- Nail psoriasis - this can happen with or without the accompaniment of the typical psoriasis skin rash. The nails look like they have little pits in them and are crumbly.
- Scalp psoriasis - on the head
- Erythroderma - all-over body redness that is life threatening (very rare)
Potential complications of psoriasis
30% of people with psoriasis will go on to develop psoriatic arthritis2. This a painful inflammatory condition of the joints, that may come on 5 to 10 years after the initial psoriasis rash begins. It is also possible to develop psoriatic arthritis without having the skin signs. The things to look out for are:
- Painful and swollen joints (typically knees, ankles, feet and hands)
- Pain over tendons in the body (such as the achilles tendon at the back of your ankle or plantar fascia on the bottom of your foot)
Links have been found between psoriasis, anxiety and depression. Although some might feel depressed or anxious because of their psoriasis, the relationship between mental health and this skin condition are more complex than that. Stress and depression have been considered triggers to psoriasis, and vice versa. It is incredibly important to speak to your GP if you are suffering from anxiety [link to anxiety] or depression [link to depression], as help with your mental health might also help your psoriasis.
There also appears to be a link between psoriasis and other health problem such as irritable bowel syndrome, cardiovascular disease, metabolic syndrome and deep vein thrombosis (blood clots). If you have psoriasis, your GP will monitor your cardiovascular health every 5 years but it is a good idea to read around psoriasis as much as possible so that you know how to keep your risks of these associated conditions as low as possible.
How does a GP diagnose psoriasis?
Psoriasis is usually quickly diagnosed by showing the rash to a GP and it can be diagnosed via a digital video consultation. The rash looks very different from other common rashes, such as eczema.
There is no test that confirms psoriasis. If your GP is unsure, they might offer you an appointment in clinic or you may be referred to a dermatologist (a doctor who specialises in skin conditions).
What treatment options are there?
Treatment is aimed at reducing the inflammation of the skin in order to try and reduce (or sometimes clear up) the rash.
Unfortunately psoriasis is a chronic skin condition that comes and goes and is not usually curable, but the good news is that it can often be improved.
The treatment your GP will prescribe depends on the type of psoriasis you have and where the rash is on your body. In brief, the treatment options can be divided into:
- Creams (i.e. steroids, vitamin D analogues, calcineurin inhibitors, coal tar and moisturisers)
- Light therapy (PUVA, UVB)
- Oral/injected medicines (i.e. methotrexate, ciclosporin, retinoids, biologic therapy)
To speak to one of our GPs, download the app and create an account today.
Other things you can do to improve psoriasis
Studies have shown that psoriasis is worsened by the following:
- Smoking
- Drinking excessive amounts of alcohol
- Being overweight
Have a look at this excellent Psoriatic Lifestyle and Nutrition Guide from the Psoriasis and Psoriatic Arthritis Alliance, which gives advice around how you can improve psoriasis through changes to your diet and lifestyle.
More information
The Psoriasis and Psoriatic Arthritis Alliance - www.papaa.org
The Psoriasis Association - www.psoriasis-association.org.uk
NHS - www.nhs.uk/conditions/psoriasis/
References
- Parisi,R., Symmons,D.P.M., Griffiths,C.E.M. and Ashcroft,D.M. (2013) Global epidemiology of psoriasis: a systematic review of incidence and prevalence. Journal of Investigative Dermatology. 133(2), 377-385.
2. NICE Psoriasis [online] Last updated March 2018. Accessed 8/3/2019. https://cks.nice.org.uk/psoriasis/
The information provided is for educational purposes only and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Seek the advice of a doctor with any questions you may have regarding a medical condition. Never delay seeking or disregard professional medical advice because of something you have read here.
